A New Framework
After Nandi and Puranam introduced her to the field of trauma-informed care, Elisseou began to assemble her physical exam maneuvers into the standardized framework she would ultimately teach in the Doctoring course. Though the concept of trauma-informed care has been around for decades, such a specific framework, focused on its application to the physical exam, did not exist. Elisseou’s framework includes specific language and behaviors to employ before, during, and after a routine medical exam in order create a safe environment and avoid triggers of prior trauma.
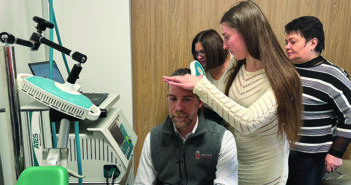
For example, in a traditional thyroid exam a physician will stand behind the patient, outside of the patient’s field of vision, and wrap their hands completely around the patient’s neck. Such a maneuver can trigger sensations of violent choking, she says. “This instead can be done with the practitioner standing at the patient’s side, within their eyesight, with the fingers extended, the thumbs away from the neck, and saying to the patient: ‘I am going to place my hands on the neck in order to examine the thyroid. When you can, please swallow,’” Elisseou says. “This lets the patient know exactly what you’re doing and why, and it avoids the sensation of choking.”
Elisseou’s thyroid exam highlights some of trauma-informed care’s basic tenets: remaining in the patient’s field of vision; explaining the procedure and its purpose clearly; and employing maneuvers that are intentional and sensitive to the feelings they cause.
Similarly, Elisseou says having patients sit slightly upright during a pelvic exam both minimizes the patient’s physical vulnerability and allows them to maintain visual contact with the provider.
She also emphasizes the deliberate use of language in creating a trauma-informed atmosphere during the examination. “We hear physicians and trainees say ‘for me’ all the time when they’re giving patients instructions,” Elisseou says. “Sometimes this phrase can enhance the power differential between physician and patient, and can even, in certain cases, be sexually suggestive and inappropriate. For example: ‘swallow for me,’ ‘bend over for me,’ ‘lower your gown for me,’ ‘take off your shirt for me.’” She instead refers to parts of the patient’s body using the article “the,” rather than the more personalizing “your.” “It feels different to hear, ‘I’m going to look at your vagina,’ versus ‘I will now inspect the vagina,’” she says. She gives clear explanations and instructions as another way to enhance the patient’s feelings of safety, autonomy, and trust.
In spring 2017, Elisseou introduced her framework to students in an optional workshop, with hands-on practice. Student feedback was overwhelmingly positive. Sukrit Jain ’16 MD’20 says the workshop made him aware of his body positioning and language choice during patient encounters. “I always place myself in the patient’s line of sight now, and I try to inform my patients of the reasons behind my physical exam maneuvers,” he says.
Nandi, Puranam, and Elisseou were moved by such responses. “We’ve been so humbled by our peers, our colleagues,” Puranam says. “People we respect and look up to are finding value in this. It shows that our medical community is seeking a framework like this.”
The team is also excited about the potential of this framework to help providers cope with some of the insidious challenges of practicing medicine. A 2011 meta-analysis published in Academic Medicine found that students enter medical school with, on average, more empathy than the general population. Four years later, after completing undergraduate medical training, they are less empathetic than their peers outside of the medical world. More than ever, physicians identify the broad notion of “burnout” as the enemy of empathy. Elisseou sees a framework for trauma-informed care as a potential antidote. “I think that burnout inhibits our function on many levels,” she says. “However, when empathy is hard to call up and compassion is hard to find, we can rely on learned skills in the form of a trusty framework or a checklist that can still get the message across.” Puranam and Nandi add that helping providers better understand the contexts, histories, and environments of their patients could enable tired and frustrated students, residents, and physicians to harness empathy.
Last year Elisseou, by then the course leader for first-year Doctoring, decided to integrate trauma-informed care into the standard curriculum. She says the response has been positive: “I have gotten feedback from first-year medical students that this is an exciting subject that they look forward to practicing with patients at their mentor sites.” Vivian Chan MD’21 says that she has employed the skills she learned from that lecture during her weekly mentor sessions at the Providence VA. “It is a more empowering, and more comfortable, kind of approach,” she says.