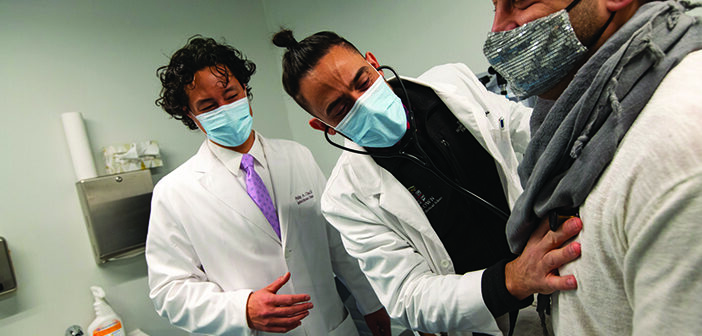
Open Door Health is lowering barriers by providing culturally congruent health care.
If the bright, sprawling mural dedicated to Rhode Island’s queer and trans communities isn’t the first thing to make a visitor to Open Door Health in Providence feel at home, they are sure to feel welcome the second they step inside the clinic’s Central Street building.
“It’s our goal to provide a warm embrace from the beginning,” says Amy Nunn, ScD, a professor of medicine and of behavioral and social sciences at Brown and a cofounder of the clinic. “We will use their preferred pronouns. Their gender expression and sexual orientation are affirmed. If they speak Spanish, we have providers who also speak Spanish. Those things may sound basic, but they’re really not done at many places.”
Those “basic” practices combined with a goal of improving health equity by connecting patient care with research is what drives the mission of Open Door Health, the first dedicated clinic in Rhode Island to provide culturally congruent primary and sexual health care to members of the state’s LGBTQ+ community.
Nunn launched the clinic with Philip Chan RES’09 F’11, MD, MS, associate professor of medicine and of behavioral and social sciences. The two work in HIV prevention and treatment, both separately and as frequent collaborators. Nunn serves as the executive director the Rhode Island Public Health Institute, which founded the clinic. At Open Door Health, Chan serves as the chief medical officer; he is also a medical director at the Rhode Island Department of Health.
“Amy and I have always worked so closely together, because we believed in not just studying critical public health issues but addressing them,” Chan says.
The inspiration for Open Door Health came from Chan’s interactions with patients receiving HIV prevention care. Even though some had primary care physicians, they felt more comfortable visiting other clinics and specialized health centers, where their sexual orientation or gender identities weren’t questioned and providers didn’t judge them for seeking pre-exposure prophylaxis (PrEP), a single pill taken once daily that prevents HIV infection.