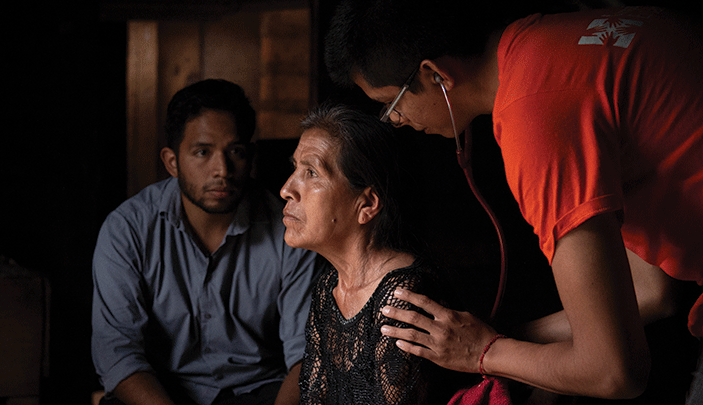In rural Mexico, physicians take care of the whole person, not just their illness.
Doctor, doctor! She is having an attack again. She can’t breathe! She can’t breathe! Come to the clinic quickly!” Argel Martínez, MD, opened the door of his humble two-room home in Chiapas, Mexico, and hurried after the family to the clinic, although it was late: already around 9 p.m. When I arrived just after, there was a young woman named Mariana (not her real name) lying on the exam table, hyperventilating and shaking intensely. The electricity in the community was out; we used a headlamp for lighting. Argel laid his hands on her sternum. He knew she was having an anxiety attack, and he knew what his treatment plan would be. It was his close relationship with the patient and her family that allowed him to make a quick diagnosis and respond appropriately.
In the hospital settings that I’m used to, this patient likely would have undergone an expensive workup (labs, EKG, imaging studies) and been medicated, with little individual attention. However, Argel was living in Plan de la Libertad for a year, and had become a part of the tiny Chiapas community. He saw not only its various cases of illness and injury but, more importantly, he saw each case as a part of an individual person’s lived experience. He didn’t simply medicate Mariana with an anxiolytic and move on to the next patient, as emergency rooms often pressure clinicians to do. Instead, with human touch, reassurance, and connection, he guided her through deep breathing and relaxation techniques for over an hour until she was breathing calmly. He assured her and her family that if there was anything else they needed, he was there for them.
In Mexico, all first-year clinicians complete an obligatory year of social service, or pasantía. Argel had chosen to do his in Chiapas because he wanted to be part of something bigger, though he didn’t yet have a name for what that was. While his medical school had trained him to diagnose and take care of diseases, they did not teach him how to take care of the whole person with that illness. He had never heard about social medicine or global health until he discovered Compañeros En Salud (CES), as Partners In Health is known in Mexico.
CES has had a reputation for providing quality primary care to patients, as well as support for its providers, since 2011. Placement in a rural clinic in Mexico is usually dreaded by young pasantes due to multiple structural problems including lack of resources, exposure to violence, poorly stocked clinic pharmacies, and the lack of a feasible way to refer patients into specialized care. Pasantes in rural areas usually do not have the opportunity to work in team-based settings, and do not have help from community health workers either. At CES, it’s the opposite. Argel knew he would not be alone. As he cared for patients like Mariana with more complex cases, he would have the support of CES’s auxiliary programs that complement the primary care he provided: maternal health care, referrals, and, in Mariana’s case, a mental health program, whose team guided her care and provided him with ongoing education.
A HUMAN RIGHT
As a second-year family medicine resident in 2017, I worked with Argel in Plan de la Libertad for one month. I supervised him in clinic and helped him expand his differential diagnosis skills. It was clear that he had an excellent foundation of knowledge, so my job was to challenge him beyond the basics. For the most part, we treated chronic diseases (such as diabetes and hypertension) and acute illness (like diarrhea) in the same way as we do in the US. He was practicing evidenced-based medicine in one of the most remote areas of Mexico. The medications available to him, thanks to CES, are similar to the ones that I have for many of my patients in the United States. When people asked, “What is it like in Chiapas?” I would tell them that my work in CES-supported clinics is similar to my work in Rhode Island in that we do the best with what we have to provide quality primary care to every patient regardless of race, class, gender, or documentation status. Argel and I shared a lot of commonalities, and we both live by Partners In Health’s belief that health care is a human right.
A year later, I came back to Chiapas as a global health fellow to help create and implement a family planning curriculum with the CES maternal health team. Working with Argel as a mentor had motivated me to become a better teacher. Argel had returned to CES, too. He’s now a clinical supervisor for three CES pasantes in the rural communities where they live and work. He helps troubleshoot complex cases, provides direct supervision in clinic as a mentor, and facilitates referrals for patients needing specialized care.
When Argel first came to Chiapas, he didn’t have a word to describe what he wanted to be as a physician. Now he does: acompañate. It doesn’t quite have an English equivalent. We use acompañates to describe the community health workers at CES, who truly walk side-by-side with our patients, who build relationships with them and their families. Argel knows he wants to always be there for patients like Mariana, for the young physicians he supervises, and for his colleagues. He wants to be their acompañate.