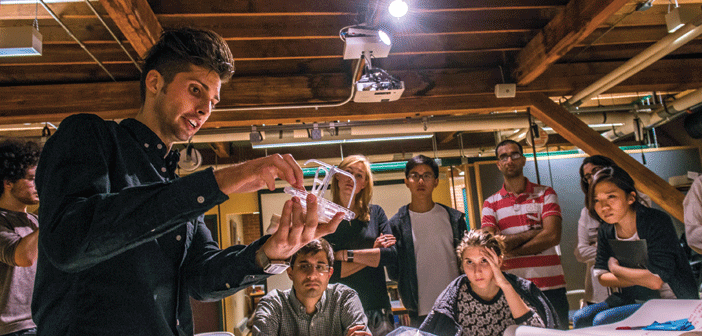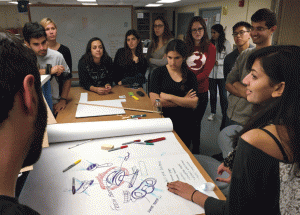Brown and RISD students take a fresh look at health care problems.
User friendly, affordable, efficient: they’re adjectives few people associate with health care—physicians included.
From electronic medical records to isolation gowns to procedure tables, providers want more functionality and improved outcomes. In most cases, that means better design. Yet designers, who possess the imagination and the prototyping skills, have little access to or knowledge of the world of medicine.
Ravi Sarpatwari MD’16, who studied architecture before coming to Alpert Medical School, wanted to bridge this divide. With guidance from his scholarly concentration adviser, Jay Baruch, MD, associate professor of emergency medicine, Sarpatwari teamed up with three Rhode Island School of Design students in 2013 to create an elective for students of both schools where their combined talents could, potentially, change the world of health care.“A lot of companies are thinking about how design can support health care,” Sarpatwari says. “But educationally there aren’t a lot of opportunities to teach that.”
The preclinical elective, Design + Health, proved popular with students, faculty, and even some local industry and community leaders, who presented problems at workshops and mentored students as they brainstormed solutions, built prototypes, and presented their concepts to a panel of critics in the final class.
Pranav Reddy MD’17, whose group that year envisioned a more transparent, easy-to-use EMR, says it was “by far” his favorite elective. “After taking it, I was able to see familiar objects in the health
care setting in unfamiliar ways,” he says. Inspired, Reddy took a lead role in the course last fall, working with Sarpatwari; Baruch, the faculty adviser; and other medical and RISD students and faculty to build on the pilot’s success. They got a grant from Brown’s Creative Arts Council, as well as the participation of more departments and nonprofits.
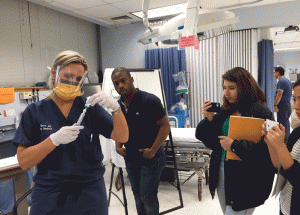
Jessica Smith, MD, associate professor of emergency medicine (clinical), demonstrates ED procedures in the Lifespan Medical Simulation Center. (Credit: Pranav Reddy)
“If the doctor is balancing things on the patient, it doesn’t instill confidence,” Baruch says.
Leo Kobayashi ’94 MD’98, associate professor of emergency medicine, and Tony Zhang, MD RES’17 had begun designing a prototype table that could clamp to the side of a gurney, but wanted
to make it adjustable and easier to use. Their workshop inspired RISD student Aimee Kim to choose the project. “I was able to see how it could be so much better, from an outsider’s and a designer’s perspective,” she says.
Ana Bermudez ’12 MD’18 found broader lessons as she worked with her RISD teammates on the procedure table. “In design, every failure is important because it tells you how to do better,” she says. “Medicine only improves and grows from looking at non-successful instances.”
One aspect of the course frustrated nearly everyone involved: lack of time. At the final class, none of the four groups had a fully functioning prototype to present, and their lists of “next steps” were extensive, including more research, product trials, and gathering user feedback. Bermudez and Kim’s group showed only photos of their model; another group, which designed a simpler isolation gown, displayed tiny, doll-size gowns and played a video to demonstrate donning and doffing technique.
The critics, including a RISD industrial design professor and local health industry representatives, questioned each group closely about cost, materials, and existing alternatives to help them hone their products, and presentations, in anticipation of a real-world launch. Reddy and Sarpatwari say they hope to find funding so at least one group can try to bring their project to fruition.
One critic, Sandra Potter, PhD, a start-up adviser at MedMates, a local health care technology networking group, told the students the semester-long course represents only the first step of the design process. “We need a phase two of this class, to take this thing further,” she says.