New technologies prevent drug-resistant pathogens from taking root.
Scientists and clinicians have been ringing alarm bells about antimicrobial resistance for decades. Yet as more and more “superbugs” repel more and more treatments, and more and more people die—at least 1.27 million in 2019, according to The Lancet—governments have done little to incentivize the development of new drugs by the public or private sector.
The most terrifying pathogens aren’t just multidrug resistant, they’re pan resistant: impervious to all known antibiotics. While doctors’ drug arsenals desperately need a boost, some researchers are focused on preventing infections before they start.
“At some point there’s nothing left,” says Dioscaris Garcia PhD’12, a microbiologist and assistant professor of orthopaedics (research). “You need something that is going to uncouple that cycle of, new antibiotic comes in, bacteria mounts a resistance, and then we’re back to square one.”
Garcia is a co-director of the Diane N. Weiss Center for Orthopaedic Trauma Research at Rhode Island Hospital, where he and co-director Christopher Born, MD, are developing technologies to stop bacteria from adhering to orthopedic implants, infiltrating wounds, and colonizing prosthetic liners. They’re also trying to speed up diagnosis with a test that locates and identifies offending microbes in minutes instead of days.
Born, a trauma surgeon and the Intrepid Heroes Professor of Orthopedic Surgery, began working years ago on a previously patented antimicrobial coating “weaponized” with silver carboxylate to reduce the formation of layers of microbes known as biofilms on surgical screws, catheters, and other hardware. “[Biofilms] are relatively impermeable to antibiotics and other means,” Born says. When they form, surgeons must remove the infected implant, clean the area as best they can, administer antibiotics, and hope for the best.
In published and recently submitted studies, Born, Garcia, and co-authors have shown that a silver carboxylate coating inhibits biofilm formation by Acinetobacter baumannii, Enterococcus faecium, and methicillin-resistant Staphylococcus aureus—three of the bacteria on the WHO’s “priority pathogen” list.
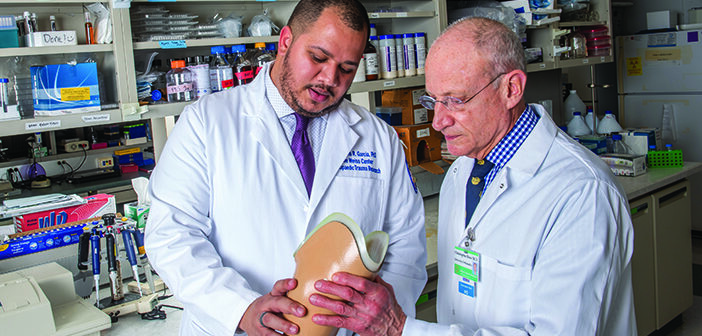
While Garcia and Born need FDA approval before this coating can be applied to implants in humans, it’s already in use on prosthetic liners, where it prevents not only skin inflammation and irritation, but also odor caused by the breakdown of bacteria, Born says. “This is a big complaint that people who have limb loss talk about, but have not been open about,” he adds.
The team also has patented technology to more rapidly identify pathogens when infection sets in. Current tests can take up to two weeks to return results; clinicians are forced to either guess which drugs to administer, or use broad-spectrum antibiotics—and further contribute to antibiotic resistance. The Weiss lab’s rapid visualization assay (RVA) uses immunofluorescence and microscopy to detect the same bacteria that existing technologies do, but in just half an hour, Born and Garcia say.
Garcia says the RVA device—which “looks just like a Keurig”—could offer “point-of-service infection detection.” A surgeon can remove a piece of hardware or a bit of tissue or joint fluid, place it in the visualization chamber, and in about 30 minutes identify and quantify the bacteria present. “You see exactly where the infection pockets are,” Garcia says, and remove the microbes “with a targeted irrigation.”
Best of all, the assay can be done for as little as $1. “If you’re in a third-world country, if you were in the middle of a war theater, you may not give a darn how many bacteria you have in there, you just want to know if there’s bacteria in there,” Garcia says. “The system was designed with that flexibility in mind.”
The technology is ready for licensing. Yet even before COVID, it was difficult to garner commercial interest. “Know any people who are in the angel funding world?” Born says with a rueful laugh. “This is real. It works. It’s quite remarkable.” Until they find an interested financial partner, Garcia says, they’ll keep trying to improve it, to perhaps make it even faster or incorporate artificial intelligence. Because the threat of antimicrobial resistance will only continue to grow.
“Until COVID came around, this was one of the top priorities for the World Health Organization,” Garcia says. “We now are in dire need of having a technology that stays one step ahead.”