We know the stats. But what are we doing to improve women’s health?
Growing up in northern Ghana, Methodius Tuuli, MD, MPH, MBA, knew of too many women who suffered from pregnancy complications, and too many newborn babies who died. He saw the challenges his own mother and his four sisters faced trying to get good medical care. The experiences propelled him to the University of Ghana Medical School and a career in obstetrics and gynecology.
When Tuuli left his home country for Atlanta in 2004, to begin his residency at Emory University, he thought he was also leaving behind distressingly high maternal and fetal mortality rates. “I thought, oh, these are developing country problems,” Tuuli says. “And you come to the US, and some days I’m reminded that this looks like what it was in Ghana.”
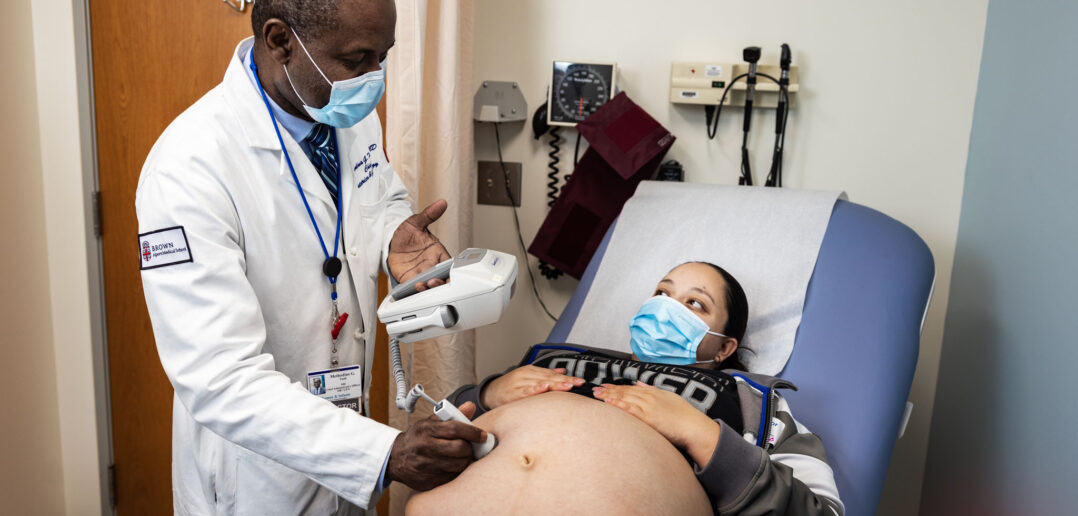
Women & Infants Hospital, where Tuuli is chief of obstetrics and gynecology, is by far the largest obstetrical facility in Rhode Island; about 80 percent of babies in the state are born there, and the patient population reflects that diversity.
Unfortunately the Ocean State also mirrors nationwide rates of poor maternal and infant outcomes—not as high as Ghana’s, to be sure, but significantly higher than peer countries like Japan, Australia, New Zealand, and most of Europe.
“Although the US is a developed country, our outcomes, in terms of maternal morbidity and mortality, are near third-world-country level,” says Tuuli, who is the Chace-Joukowsky Professor and Chair of Obstetrics and Gynecology. “And part of the reason is that we have disparities in outcomes, with Black and brown patients having much worse outcomes than our white patients.”
In Rhode Island, fortunately, the number of pregnancy-related deaths each year is too low to identify trends by race and ethnicity. However, other differences are clear: for example, while in 2020 the state had an overall infant mortality rate of 4.2 per 1,000 live births, according to the 2022 Rhode Island KIDS COUNT Factbook, 9.8 Black babies out of 1,000 died before their first birthday. That’s more than three times the rate that white infants died, and nearly twice the rate of Hispanic infant deaths. Rates of preterm births and low birthweight also show significant racial and ethnic disparities, and patients of color are more likely to receive delayed prenatal care than are white patients.
Several years ago, Women & Infants, in partnership with Brown’s Department of Obstetrics and Gynecology, began taking steps to address these inequities. From implicit bias training for all staff, to courses on racism in the residency curriculum, to a specific focus on social determinants of health in all case reviews, to a concerted effort to build a more diverse workforce, the changes have been sweeping, touching every employee and every aspect of ob/gyn care. Substantially improved patient outcomes, however, are only just starting to materialize—as Tuuli readily admits.
“The hospital and health system leaders are committed to this work,” he says. “It’s difficult, and some of these interventions won’t work. If it were easy, people would have done it already, right? … I’m just glad that we are starting.”
Founded in 1884 as the Providence Lying-In Hospital, Women & Infants has expanded far beyond its original, exclusive purpose as a facility for labor and delivery. While obstetric care remains its bread and butter, providers there treat patients from puberty through menopause. The hospital has strong programs in pelvic floor medicine, oncology, and reconstructive surgery. Patients can see reproductive endocrinologists and infertility specialists, and receive care for high-risk pregnancies and psychiatric conditions. There’s a busy emergency department and the only newborn intensive care unit in the region.
Less visible to the general public, but underpinning all of this clinical work, is a robust research program, a partnership with Brown and the Medical School. “There is a blossoming research portfolio,” Tuuli says. They are members of exclusive groups of academic research centers like the National Institute of Child Health and Human Development’s Pelvic Floor Disorders Network, Neonatal Research Network, National Cancer Institute-funded NRG Oncology, and Maternal-Fetal Medicine Units Network.
“We count ourselves very lucky to be part of this select group at the forefront of answering y critical questions that go on to change practice,” Tuuli says of the MFMU Network. “Many of the trials that have been done within this network—some led by our very own Dwight Rouse [MD, MPH, professor of obstetrics and gynecology]—have changed how we take care of pregnant women and newborns.”
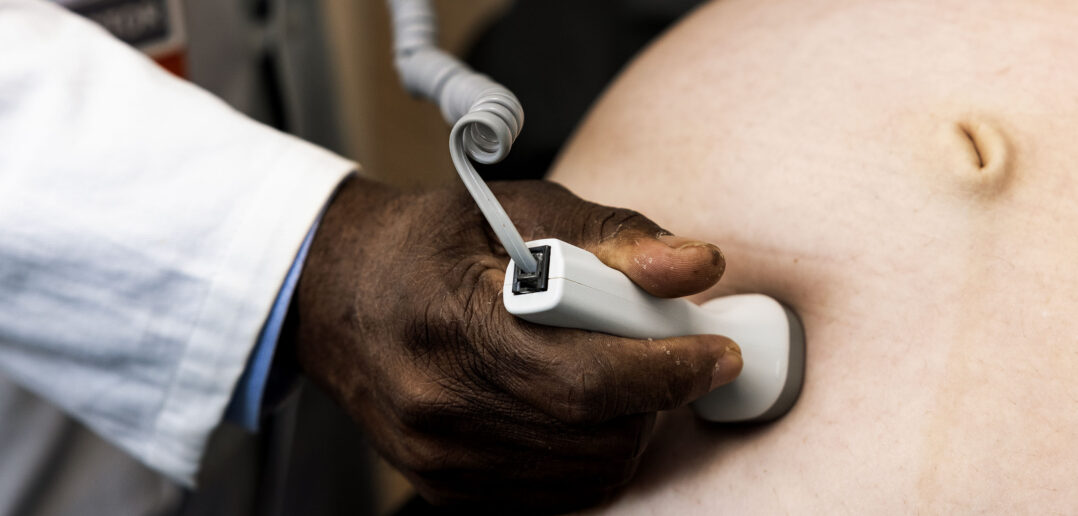
“Advances in technology have really benefited our field,” he continues. Ultrasound, for example, has progressed so much that specialists can identify and treat problems—even perform surgeries— before babies are born. Diagnosis of genetic conditions in utero no longer requires a risky amniocentesis, Tuuli adds, but a sample of blood from the mother, which carries the fetus’s DNA. “And now we are moving to the next stage, where we are attempting to sequence the whole genome of the baby from the mother’s blood,” he says.
Such progress only underscores how much work needs to be done. “The opportunities are plenty. There are still many fundamental complications of pregnancy we don’t fully understand,” Tuuli says, like preterm birth and preeclampsia. Though babies born as early as 23 weeks have a better chance now, he says, “we still don’t understand these two big syndromes enough to be able to prevent them.”
Health disparities exacerbate these challenges. “Most of the complications we are trying to prevent are more common in our Black and brown patients,” Tuuli says—30 to 50 percent more than in white patients. Therefore, researchers not only design studies to include a representative sample of the population, they also analyze the data to ensure an intervention is improving outcomes for all patients and reducing disparities.
“We are lucky to cater to 80 to 90 percent of the women in Rhode Island,” Tuuli says. “I think there’s probably no other state where one hospital can say they care for such a large proportion of the state’s population, which means the work we do here can have a true population impact.”
Paul DiSilvestro RES’94, MD, the director of the Program in Women’s Oncology and the Division of Gynecologic Oncology, returned to Providence in 2003 after his fellowship at the University of Oklahoma and several years on the faculty at Stony Brook University. When asked of his work in the smallest state, “Do you really see the gamut of gyn cancer, at least as it’s represented in the US?” he replies, “We’ve seen it all. We have such a broad mix here, from a socioeconomic and ethno-cultural perspective, and the risk factors you see with different malignancies.”
DiSilvestro, a professor of obstetrics and gynecology and an ovarian cancer researcher, helped to further develop and expand the clinical trials research program in Women’s Oncology at the hospital. He says one of the program’s priorities is “clinical trial access for every single person who walks through our door.” Brown and Women & Infants are part of NRG Oncology, a research group with members around the world, and the second-leading recruiters nationally to NCI gynecologic oncology studies within this system.
“Little known fact—Little Rhody representing out there,” DiSilvestro says. “But that’s a direct result of people being committed to the idea that these are important for not only our patients, but for all women cancer patients in general.”
There’s always room for improvement, however. The program is looking at the diversity of participants in their clinical trials and whether they represent a disease’s expected patient population. For example, “if the people that are affected by a cancer are 80 percent non-Hispanic white and 20 percent Black, then you should have that ratio in your trial enrollment,” DiSilvestro says.
Due to the history of racism, coercion, and abuse in medical research, many people are understandably hesitant to join studies, DiSilvestro acknowledges. “You have to understand that when speaking to people,” he says. “You essentially have to make very clear from the beginning that this is an option for you—in no way do you have to do this, and I will still be your provider.”
DiSilvestro is excited about several ongoing trials, including three related to immunotherapy. In September he was the lead author on a study that found a “tremendous overall survival benefit” from an ovarian cancer drug, he says. It was especially thrilling because so few trials are positive.
“But when you do hit one, the joy that comes out of it is being able to sit down with a patient who fits that diagnostic criteria and say, ‘I’ve got something really exciting to offer you,’” DiSilvestro says. “When you can actually yield an outcome that’s a direct benefit to a patient with cancer—that’s the real payoff in all of this.”